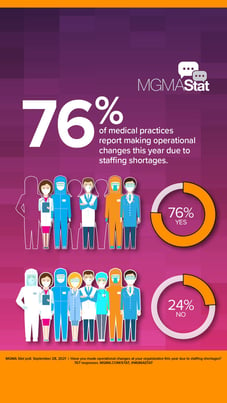
73% Of Medical Practices Rank Staffing as Their Biggest Pandemic Challenge Heading Into 2022.
An advantage of outsourcing RCM is avoidance of the high cost of staff turnover. High cost of staff turnover exacerbates healthcare industry's compressed revenue. Medical practices and healthcare organizations face a troubling revenue outlook. They deal with ever-escalating costs, which now include COVID-19 pandemic-related expenses such as additional personal protective equipment and extra sanitizing measures. At the same time, patient volumes for elective procedures and preventative and routine care remain lower than the pre-pandemic normal. On top of that, patients impacted financially by the pandemic often struggle to pay for their portion of care, upending medical billing collections.
With revenue being squeezed at both ends, it takes a significant toll on the bottom line. An AMA survey found that physician practices reported an average 32% drop in revenue last summer due to COVID-19. Another report revealed that hospital operating margins in 2020 were down 55.6% without the relief provided through the CARES Act and 16.6% with it. Check out the COVID-19 financial impact on the average physician practice versus the impact on Revele clients.
One particular, expense-side driver exacerbating this negative revenue trend is the high rate of staff turnover, which comes at a steep cost to healthcare-related films.
The Great Resignation's Impact on Overall Employment
Help wanted signs are everywhere, and job boards post new opportunities by the hour. Is it any wonder that employees are leaving their existing jobs in droves? Whether it's for higher pay, better hours, or more perks, it's easier than ever for employees to turn in their notice. In fact, that's exactly what more than 19 million people did between March and July 2021, according to the Bureau of Labor Statistics. That's an average of close to four million people quitting their jobs in each of those months.
The Troubling Turnover Rate Among Healthcare Staff
Employees in the healthcare sector made up close to 13% of the 19 million people who quit their jobs during that five-month period. Only three industries made up a larger percentage than healthcare: food services, professional business services, and retail trade.
What's more, as of August 2021, the unemployment rate in the Healthcare and Social Assistance sector was a 3.9% versus the overall unemployment rate of 5.2%. There was an even larger gap in the Hospital subsector, where the unemployment rate was just 2.7%.
Of course, turnover among healthcare staff isn't a new phenomenon brought on by the pandemic. It's an issue that medical practices and hospitals have been dealing with for years. A 2018 report by the Medical Group Management Association (MGMA) showed that primary care single specialties were experiencing significant turnover rates in several staff categories, including those related to medical billing and revenue cycle management (RCM):
- Business operations support staff: 9.92%
- Clinical support staff: 15.83%
- Front office support staff: 20%
As for hospitals, the 2021 NSI National Health Care Retention and RN Staffing Report, compared annual turnover rates for all hospital employees from 2016 to 2020. The annual rates consistently exceeded 15% and in every year but one, they veered closer to 20%.
- 2016: 16.2%
- 2017: 18.2%
- 2018: 19.1%
- 2019: 17.8%
- 2020: 19.5%
That amounts to an accumulated 5-year turnover rate of 90.8%.
The Cost Burden of Healthcare Staff Turnover
Over the years, experts have tried to quantify the financial impact of healthcare staff turnover. As far back as 2004, an analysis of turnover cost in a major medical center estimated that, at a minimum, it "represented a loss of >5 percent of the total annual operating budget." In 2018, MGMA noted that, "the cost to replace a member of management can be as high as five times their yearly salary. To replace even an entry-level employee can cost up to 25 percent of an employee's salary."
More recently, a healthcare placement firm cited a study that estimated that a healthcare provider with 300 employees and an annual 10% staff turnover rate could expect that to cost it approximately $2 million. Translate that to practices or organizations with staff turnover rates near the 19.5% average for hospitals in 2020, and it equates to an even bigger bite out of the bottom line.
The costs related to staff turnover fall into the following categories:
Direct Costs of Staff Turnover
When an employee leaves a medical practice or a healthcare organization -- whether they are a nurse or medical assistant or they are the person who manages the medical billing or inputs data into a system like eClinicalWorks, the firm incurs several costs directly related to their departure and replacement:
- Termination: This can include staff time to do things like conducting an exit interview, collecting company-issued equipment or property, and adjusting payroll and benefit systems. If the exit is an involuntary one, even more staff time is required.
- Recruitment: Finding a suitable replacement means arranging for a new job posting and sourcing, screening, and interviewing appropriate candidates.
- Onboarding: Once a candidate is selected, background checks, drug tests, and other HR processes must be completed.
- Orientation: New employees need to be trained on all policies, procedures, and systems that correlate to their roles. Electronic Health Record training for new staff can be expensive in terms of extra costs and time requirements of other staff assigned to train new staff.
- Staff overtime or temp pay: During the termination of an employee and while the recruiting, onboarding, and training of their replacement occurs, either other staff members need to work overtime to handle the extra workload or a temp worker needs to be brought in to do it.
Tangential Costs of Staff Turnover
Additionally, several indirect costs associated with staff turnover wreak further havoc on the revenue cycle management for medical practices and health organizations:
- Lapse in the continuity or quality of care
- Damaged reputations
- Higher accident rates
- Greater staff dissatisfaction and absenteeism
- Less productivity
- Loss of expertise and workflow experience
- Lost opportunities to bring on new patients or to deepen relationships with existing ones
MGMA's Workarounds for Worker Shortages: 8 Strategies for Pandemic Staffing Issues in Medical Practices
Chris Harrop at MGMA wrote a fantastic article about increasing problem of staffing issues -- especially related to the effects of COVID. Chris says, "Amid worker quarantines, resignations and vaccine refusals, last week’s MGMA Stat poll found that nearly three in four medical practices rank staffing as their biggest challenge heading into 2022." That's roughly 75% of all medical practices. Not only do staffing issues have a negative affect on the internal efficiency of a practice, sometimes practices are forced to turn patients away, because they simply cannot provide care for patients due to these staffing issues.
Chris offers 8 specific strategies for managing practice staffing shortages.
- Getting more out of your remaining providers and staff.
- Adjust operating hours/patient access and provide cross-coverage when possible.
- Reduce services.
- Cross-train, redesign jobs and reorganize departments.
- Outsource and automate.
- Redesign your services and centralize what you can.
- Embrace Telehealth again.
- Broaden your recruitment and hiring.
Identifying and Understanding the Root Causes of Burnout
In his article, Chris also talks about identifying and understanding burnout whether it's caused by pandemic stressors, vaccine hesitancy, requirements, and mandates, or something else. Chris includes a great quote from Jeff Comer, PhD, MHA, FACHE: "We all get burned out; you’re not alone. … Burnout happens, but the key is not to let it become chronic burnout, that it starts to affect your performance and your overall life,” Comer said. “If you’re burned out, get some help, have somebody work through with you.”
Burnout and staffing issues can go hand-in-hand. If you take burnout seriously in your practice, and really try to reduce burnout in your employees, it can have a positive impact on reducing staffing issues. Our experts here at Revele have published several articles specifically on Recognizing the Signs of Physician Burnout and 3 eClinicalWorks Features to Combat Physician Burnout.
RCM Outsourcing: An Affordable Solution
When it comes to front-office and back-office functions, medical practices have an alternative to dealing with the constant frustration and high cost of employee churn. Outsourced medical billing has been shown to be both less expensive and more accurate than in-house RCM setups. In fact, in-house attempts to ensure accurate reimbursements cost as much as 14% of total collections.
Download our free In-house vs Outsourced Medical Billing Cost Analysis to compare the difference between the two and to learn more about this sustainable alternative that helps stanch the revenue bleed from staff turnover.
INTEGRATED SOLUTIONS
Conquer the New Age of RCM
Learn how Revele's EMR and RCM solutions are helping
physician groups and health systems reduce costs and increase revenue.
If your EHR system harmonizes well with your work processes, it can make things easier on your staff and ultimately on patients as well. Choosing an EHR software can be difficult for medical practices. When making the decision, a practice should consider if the EHR will help with collecting patient information before the patient enters the waiting room. An EHR is more than a software to hold patient data. A top EHR solution will help your practice achieve more accurate medical billing, improve patient engagement and communication, and share patient information with other providers.
Optimizing care requires up-to-date, accurate patient information, and efficient medical billing also depends on complete and accurate data. When your EHR system is a unified platform, claims can be submitted more quickly, be less likely to be rejected because of mistakes, and patient billing can be done expediently.