Recently, OpenNotes published an article regarding the federal rules mandating open notes. According to OpenNotes, "taking effect in April 2021, rules implementing the bipartisan federal Cures Act specify that clinical notes are among electronic information that must not be blocked and must be made available free of charge to patients. To meet the interests of some patients, the rules allow specified exceptions."
Read the rest of the OpenNotes article below:
DISCLAIMER: OpenNotes Continues to Monitor Details Affecting the Implementation of the Information Blocking Rule and May Update This Webpage on Occasion.
LAST UPDATED: March 2, 2021 For information about the ONC Program Rule in its entirety, visit https://www.healthit.gov/curesrule/
Federal Rules on Interoperability, Information Blocking, and Open Notes:
With a projected start date of April 5, 2021, the program rule on Interoperability, Information Blocking, and ONC Health IT Certification, which implements the 21st Century Cures Act, requires that healthcare providers give patients access without charge to all the health information in their electronic medical records "without delay."
Common questions about the Information Blocking rule can be found in this FAQ.
This webpage is not official technical or legal advice. State laws around data release may not supersede the 21st Century Cures Act. Consult with your organization's Health Information Management, compliance, legal, finance, and public affairs teams to find out how it applies to you.
What Notes Must Be Shared?
The eight (8) types of clinical notes that must be shared are outlines in the United States Core Data for Interoperability (USCDI) and include:
- Consultation notes
- Discharge summary notes
- History & physical
- Imaging narratives
- Laboratory report narratives
- Pathology report narratives
- Procedure notes
- Progress notes
Clinical notes to which the rules do not apply:
- Psychotherapy notes that are separated from the rest of the individual's medical record and are recorded (in any medium) by a healthcare provider who is a mental health professional documenting or analyzing the contents of conversations during a private counseling session or a group, joint, or family counseling session. Note: All clinicians and organizations are required to share medication prescription and monitoring, counseling session start and stop times, the modalities and frequencies of treatment furnished, results of clinical tests, and any summary of the following items: diagnosis, functional status, the treatment plan, symptoms, prognosis, and progress to date.
- Information compiled in reasonable anticipation of, or use in a civil, criminal, or administrative action or proceeding.
What Is the Timeline for When These New Rules Go Into Effect?
Under this new rule, clinical notes must be shared by health systems by April 5, 2021, and shared with a patient's 3rd party application ("app") that may be downloaded to a smart phone or other device by October 6, 2022.
Highlighted Regulatory Dates - Information Blocking Provisions (see full PDF).
Are There Any Exceptions to the Rules?
There are complex situations in which information can be blocked - and these are called Exceptions. Unless one of the Exceptions applies, clinical notes must not be blocked.
A group called actors are referred to throughout the rule. Actors include:
- Healthcare providers
- Health information networks or health information exchanges
- Health IT developers of certified health IT (ex: electronic health record vendors)
Featured below are the exceptions outlined by the final rule. They fall into two categories (source).
Category 1. Exceptions that involve not fulfilling requests to access, exchange, or use electronic health information (EHI)
- Preventing Harm Exception: It will not be information blocking for an actor to engage in practices that are reasonable and necessary to prevent harm to a patient or another person, provided certain conditions are met.
- Privacy Exception: It will not be information blocking if an actor does not fulfill a request to access, exchange, or use EHI in order to protect an individual’s privacy, provided certain conditions are met.
- Security Exception: It will not be information blocking for an actor to interfere with the access, exchange, or use of EHI in order to protect the security of EHI, provided certain conditions are met.
- Infeasibility Exception: It will not be information blocking if an actor does not fulfill a request to access, exchange, or use EHI due to the infeasibility of the request, provided certain conditions are met.
- Health IT Performance Exception: It will not be information blocking for an actor to take reasonable and necessary measures to make health IT temporarily unavailable or to degrade the health IT's performance for the benefit of the overall performance of the health IT, provided certain conditions are met.
Category 2. Exceptions that involve procedures for fulfilling requests to access, exchange, or use EHI.
- Content and Manner Exception: It will not be information blocking for an actor to limit the content of its response to a request to access, exchange, or use EHI or the manner in which it fulfills a request to access, exchange, or use EHI, provided certain conditions are met.
- Fees Exception: It will not be information blocking for an actor to charge fees, including fees that result in a reasonable profit margin, for accessing, exchanging, or using EHI, provided certain conditions are met.
- Licensing Exception: It will not be information blocking for an actor to license interoperability elements for EHI to be accessed, exchanged, or used, provided certain conditions are met.
Acronyms for reference:
- CMS: Centers for Medicare & Medicare Services
- EHI: Electronic health information
- EHR: Electronic health record
- IT: Information Technology
- HHS: United States Department of Health & Human Services
- ONC: Office of the National Coordinator for Health IT
- USCDI: United States Core Data for Interoperability
Check Out This Training Video Our Staff Created to Reiterate the Important Highlights of This Open Note Update:
Visit Notes Setup
To enable visit notes to comply with the Open Notes Mandate:
- Open Patient Portal Setting
- Healow > Patient Portal Settings (or)
- Admin > Product Activation > Patient Portal Settings
- Select Feature Settings from Left Bend
- Enable Visit Note
- Mark Yes
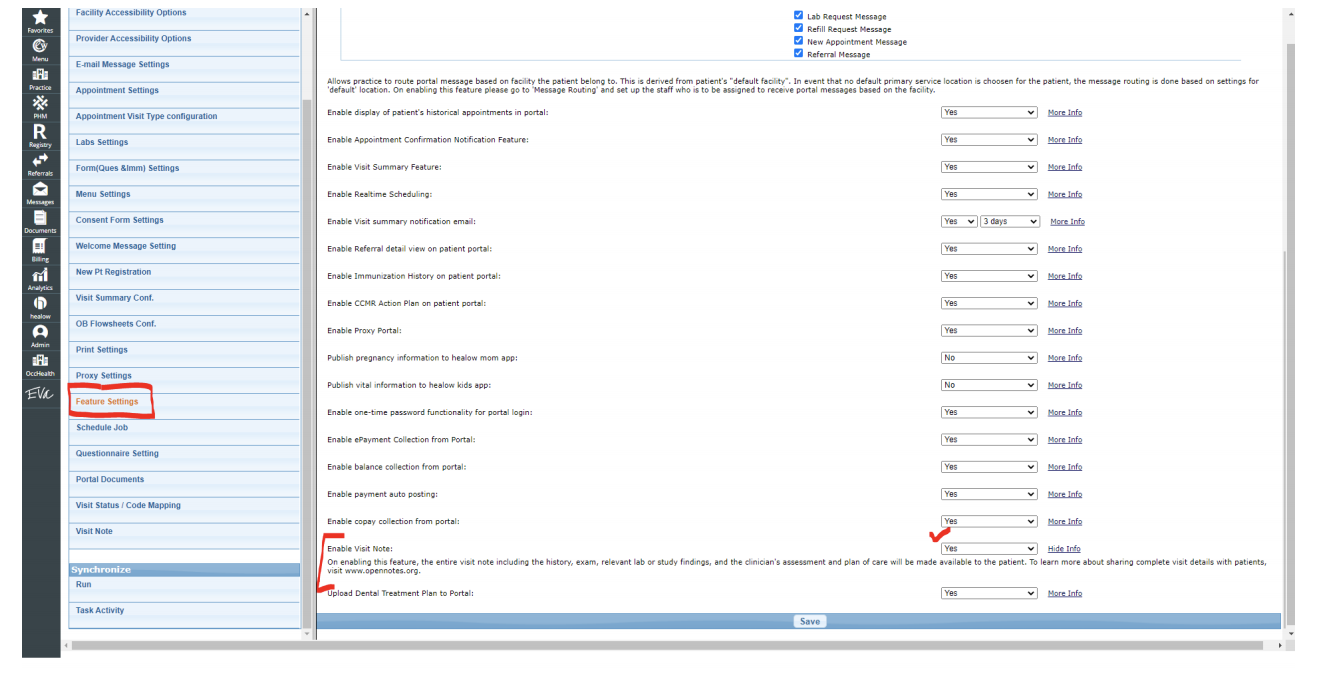
- Select Visit Note from Left Bend
- Enable the facilities that you wish to display the visit note
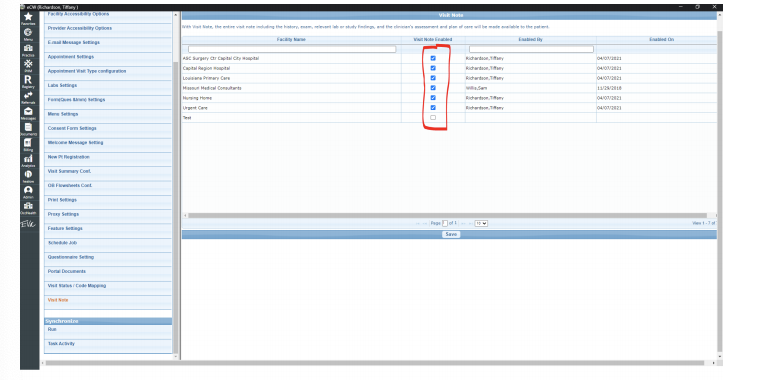
- Select Admin from the Left Navigation Band
- Select Admin again
- Select User Admin
- Select the Visit Type
- Select "Synchronize this visit type to portal"
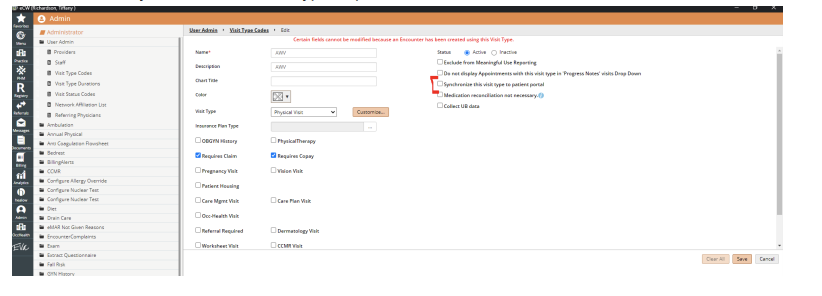
Start Date to Display Visit Notes
Healow > Patient Portal Admin Dashboard > Additional Settings > Set Date
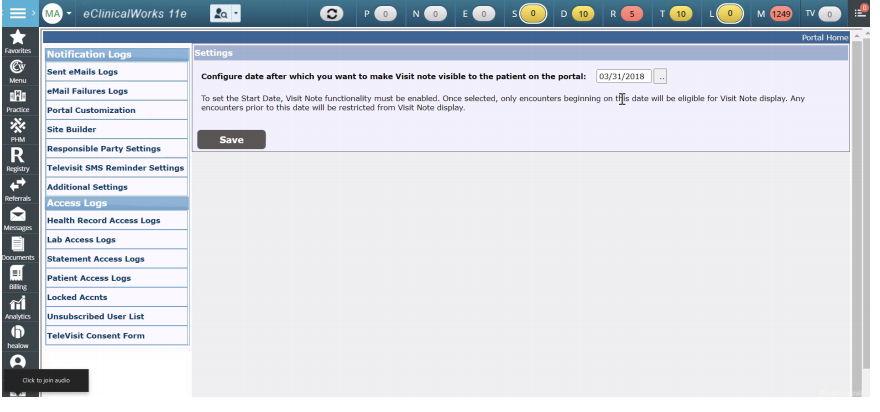
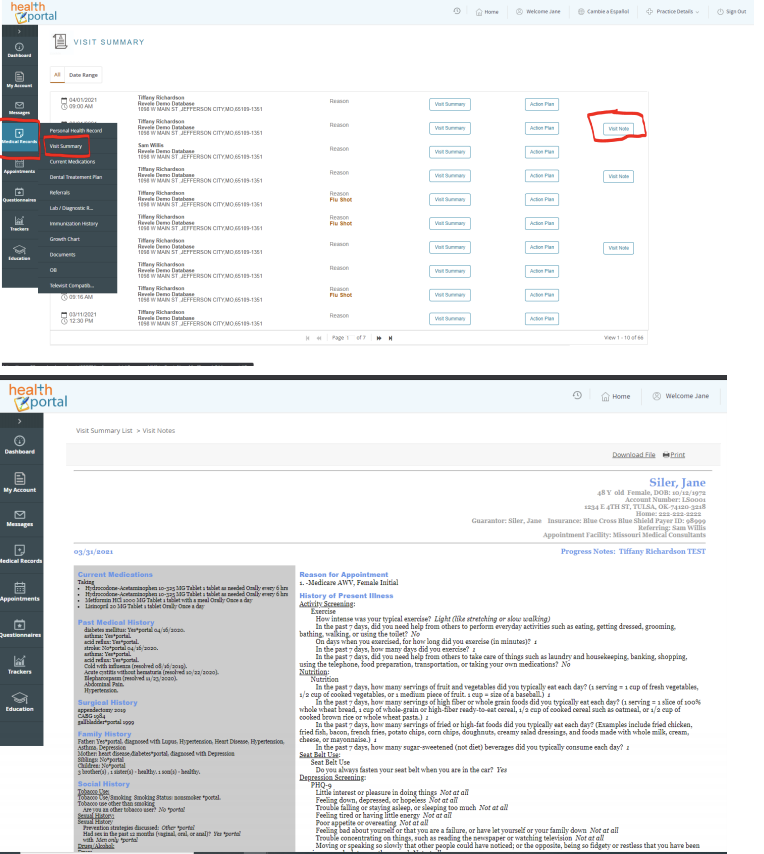
Patient Access
- Login to Patient Portal
- Select Medical Records
- Select Visit Summary
- Select Visit Note
FAQs
- What displays on the visit note?
- Everything! The system is giving the patient a copy of the locked progress note
- Does Clinical Notes display?
- Yes
- Does Visit Codes Display?
- Yes
- How do I disable Visit Codes from my progress note?
- File > Settings > Practice Defaults > Options > Deselect checkbox next to "Publish visit codes in locked progress note"
--
Further Resources
We credit the information included in this article to the writers of the OpenNotes blog and the following citations:
- This web page features content from "Federal Rules Mandating Open Notes" by OpenNotes, available under a Creative Commons Attribution 4.0 International license.
- Anonymous. (2021, March 2). Federal Rules Mandating OpenNotes. Retrieved March 30, 2021, from https://www.opennotes.org/onc-federal-rule/
- Copyright Disclaimer under section 107 of the Copyright Act 1976, allowance is made for "fair use" for purposes such as criticism, comment, new reporting, teaching, scholarship, education, and research
- Training videos and step-by-step guides created by Revele's Certified eClinicalWorks Training and Implementation Specialist Staff. 2021. Revele All Rights Reserved.