According to an article published last week by Cristy Good at MGMA, "half of practices saw days in A/R increase in 2021."
MGMA’s most recent stat poll, indicated the majority (49%) of medical practice leaders said days in A/R increased in 2021, compared to 15% who reported a decrease, and another 37% who said they stayed the same. (MGMA conducted the poll on November 9th, 2021, and had 587 responses.) Practices know that the longer a medical bill goes unpaid, the harder it is to collect. Debt.com and Forbes found that half of Americans carry some medical debt (57% owing at least $1,000).
Check out Cristy Good's article, Not-so-graceful aging: Half of practices saw days in A/R increase in 2021, for more information and a deeper explanation of all findings and recommendations.
Practices noted a few key points in the survey that added to the increase in A/R days:
- Limited office staff to work outstanding balances
- New workers face major learning curves
- Many practice leaders blamed payers for questionable denials and delays in reviewing appeals (An Aug. 24 MGMA Stat poll found 54% of medical practices reported that credentialing-related denials increased in 2021.)
Medical practices continue to experience burden by prior authorizations. (May 18 MGMA Stat poll found 81% of medical practices experienced an increase in payer prior authorization requirements in 2021.)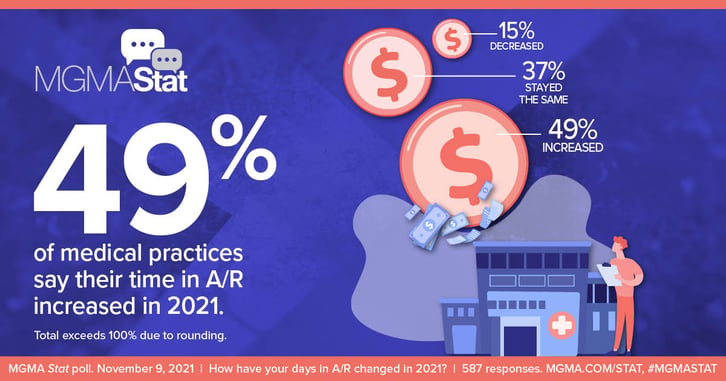
Managing Days in A/R
MGMA's calculation of days in A/R is calculated by dividing the total A/R amount by the practice’s average daily charges and is usually classified by age (the time since the patient or insurance company received billing). A/R is placed in “aging buckets” of 0 to 30 days, 31 to 60 days, 61 to 90 days, 91 to 120 days and 121+ days. According to the 2021 MGMA DataDive Cost and Revenue, the median for total A/R over 120 days in multi-specialty practices is 13.54%.
Cristy has several recommendations for creating a solid revenue cycle process including:
- Set billing guidelines and a process to collect balances due
- Establish a process for past-due accounts
- Patient communication is vital (especially if they need help to understand the portion of the bill they handle or deductibles)
- Provide payment options to help reduce bad debt and prevent debt from being sent to collections
- Run A/R reports regularly and work denials immediately
- Coding is vital for every billable aspect of your RCM process
- Staff need to be coding experts, and they should educate providers as needed
- Providers should close encounters the same day (not any longer than 72 hours after a visit)
- To learn more about Revele's expert end-to-end RCM solution, click HERE.
Check out Cristy's article for more information regarding the MGMA poll on increased days in A/R, a complete list of key items for effective A/R and improved cash flow, and more.
---
ABOUT MGMA
Overview & Mission
“We empower practices, providers, and patients to create meaningful change in healthcare.” Medical Group Management Association (MGMA) is a key element in perpetuating success throughout the healthcare industry. Whether you’re an MGMA member to advance your personal goals or your professional career, we have the resources to initiate change and drive results.
With exceptional peer-to-peer and mentor-to-peer support systems as well as abundant hard-copy and digital resources, we are spearheading the path to healthcare advancement. We are known for providing our members and the community with consistent expert resources and solutions that include, but are not limited to:
- Educational collateral and certifications
- Success strategies for students, healthcare practices, and employment needs
- Innovative ideas and networking events
- Expertly compiled benchmarking data and statistics
- Access to industry experts and thought leaders
- Information and materials for making your practice more successful and profitable
- And so much more!
end-to-end rcm solution
Demand more from your revenue cycle.
Our integrated solution brings together robust data, intelligent claim handling, and performance consulting to guarantee a 10% increase in cash flow.








