Patient-Pay
Implement a combination of modern day technologies and strategies to collect patient payments faster.
Modern-day medical billing requires multiple processes, technologies, detailed analytics and is made to be as complex as possible. We recover revenue with a systematic, individualized denial methodology that drives measurable financial improvement.
Through proven workflows, detailed performance reporting and consistent monitoring, our denial specialists are able to pursue every dollar while your staff dedicates less time to billing activities.
Achieving the shortest collection period possible means fully optimizing the features and automation capabilities available in eClinicalWorks' software. Manual processes can often lead to timely filing and missed revenue. Implementing claim automation and streamlining the communication between providers and medical coders makes claim submission quicker for faster payments.
*Source: Becker’s Hospital Review, May 2018

Constant changes to medical billing and coding can make claims management seem impossible. Revele's Certified Professional Coders utilize experience in over 30+ specialties and sub specialties to provide a range of medical coding and auditing services to assist with documentation, charge capture, and denial management.
At Revele, we're reviewing every claim and educating providers on medical coding and documentation best practice to ensure compliance and clean claims.
Practice Performance Report
As part of Revele’s holistic denial management methodology, we continuously monitor all angles of the claim process including charges, payments, contractual adjustments, write offs, and bad debt adjustments. Through ongoing monitoring and reporting, we’re able to find and fix issues affecting the claims process quickly.
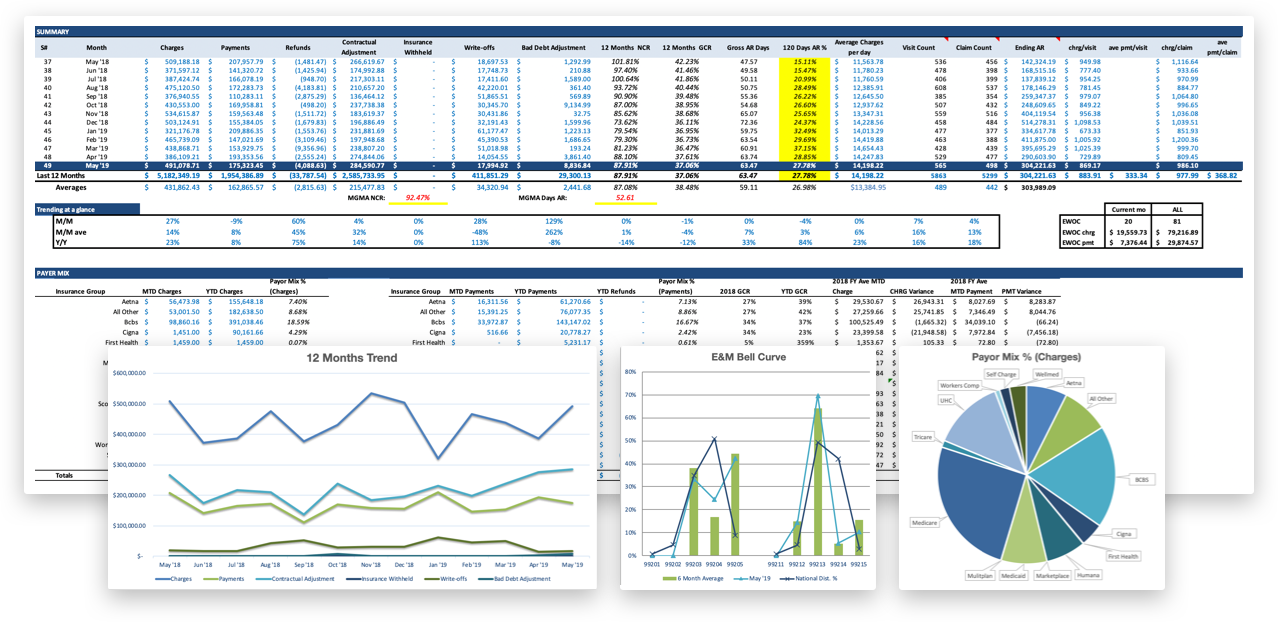
Traditional medical billing fails to think forward. The future of healthcare is changing and those that lead it need new ways to integrate data and standardize processes that span the entire claims lifecycle. That’s why Revele has reinvented the revenue cycle to enrich revenue performance for tomorrow and beyond.


©2026 Revele. All Rights Reserved.